PTBD & Biliary Stenting for Jaundice Treatment
PTBD & Biliary Stenting for Jaundice Treatment
Obstructive jaundice occurs when the normal drainage of bile from the liver to the intestine is blocked. This can happen due to stones, benign strictures or cancers involving the bile ducts, pancreas or gall bladder.
Percutaneous Transhepatic Biliary Drainage (PTBD) and biliary stenting are minimally invasive procedures that use imaging guidance to open blocked bile ducts and divert bile flow, helping reduce jaundice, itching, infection risk and improve overall condition.
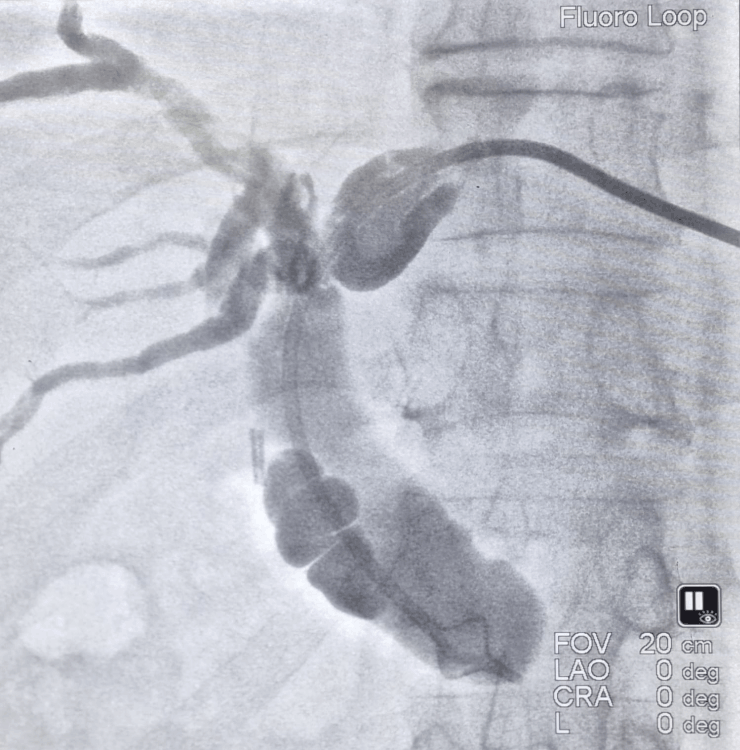
PTBD
When Is PTBD / Biliary Stenting Needed?
These procedures are considered when endoscopic methods are not possible or not adequate, or when quick relief of jaundice is required before further surgery, chemotherapy or other treatments.
The main goal is to safely drain bile, reduce bilirubin levels and relieve symptoms in patients with complex or high‑level biliary blockages.
Typical Symptoms & Situations
Patients who may benefit from PTBD or biliary stenting often have:
- Yellowing of eyes and skin (jaundice) due to bile duct obstruction
- Dark urine, pale stools and intense itching
- Recurrent cholangitis (fever with chills and abdominal pain)
- Inoperable or borderline operable biliary / pancreatic cancers
- Benign biliary strictures or post‑surgical leaks needing drainage
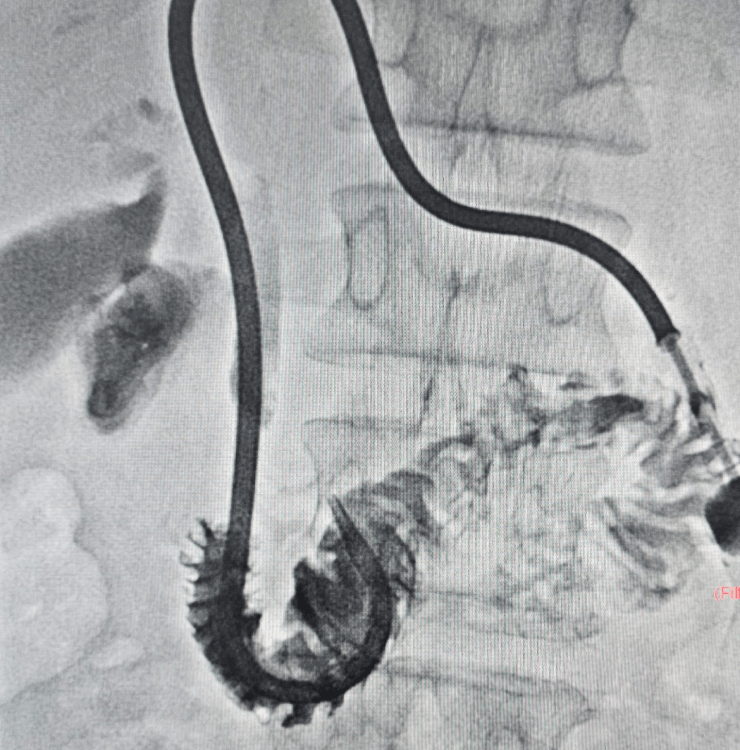
PTBD
How the Procedure Is Done
PTBD and biliary stenting are performed under ultrasound and fluoroscopy (X‑ray) guidance, usually under local anesthesia with sedation.
- Needle access into a bile duct through the skin and liver using ultrasound and X‑ray guidance.
- Cholangiogram (bile duct contrast study) to identify the exact site and extent of blockage.
- Drainage catheter placement to temporarily drain bile outside or into the intestine (internal–external drainage).
- Definitive stenting across the blockage using plastic or metal stents to restore long‑term bile flow.
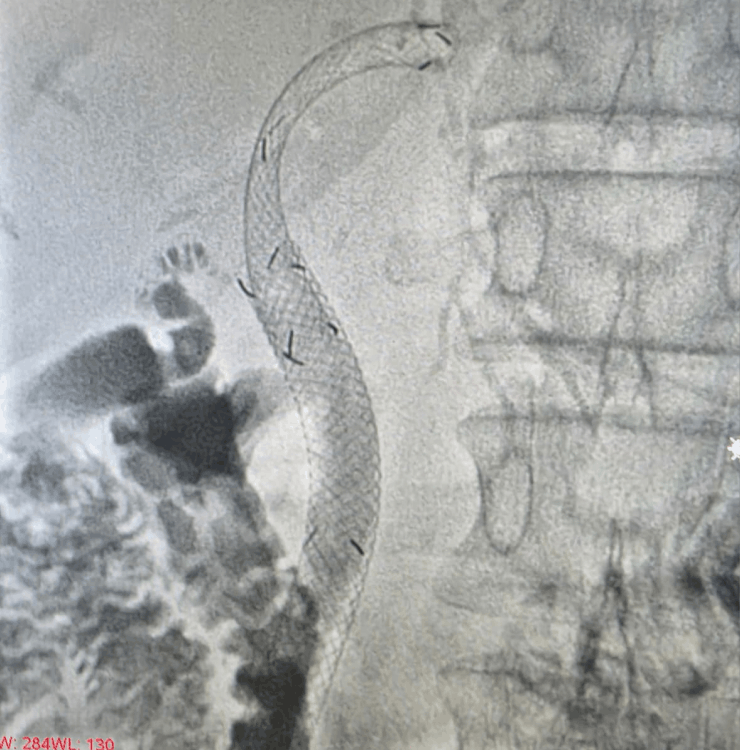
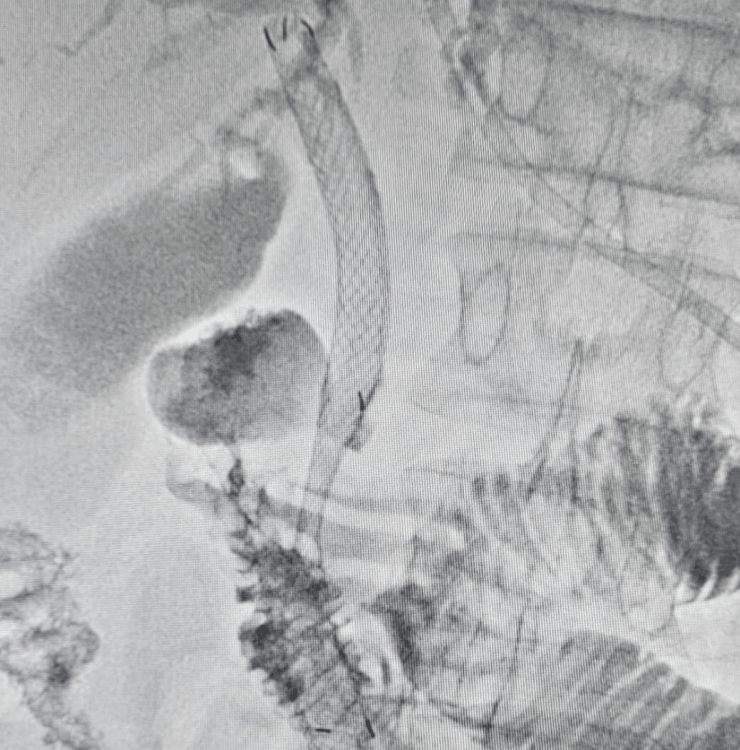
Biliary stenting
After the Procedure
Following PTBD or biliary stenting, patients are monitored and given detailed instructions for care.
- Monitoring of bilirubin, liver and kidney function tests over the next days to weeks
- Care of external drainage catheters, if present, to keep the site clean and dry
- Watching for fever, increasing abdominal pain or sudden reduction in bile output
- Regular follow‑up imaging to ensure the stent or catheter is functioning well
- Planning further oncological or surgical treatment once jaundice improves
Frequently Asked Questions
-
1.When is PTBD preferred over endoscopic stenting?
PTBD is often used when endoscopic access to the bile ducts is difficult or unsuccessful, such as in high‑level blockages, altered anatomy after surgery, or in very sick patients where a percutaneous route is safer and quicker.
-
2.Is the procedure painful?
The procedure is usually performed under local anesthesia with sedation, so you may feel some pressure or mild discomfort, but significant pain is uncommon. Pain medicines are given during and after the procedure to keep you comfortable.
-
3.How long will the stent or drain stay in place?
This depends on the underlying disease. In many malignant obstructions, metal stents are intended for long‑term use. External drains may be capped or removed once internal drainage is adequate and bilirubin levels have improved.
-
4.What are the possible risks or complications?
Possible risks include bleeding, infection, bile leak around the catheter, blockage or displacement of the drain or stent, and rarely injury to nearby organs. These procedures are performed under strict imaging guidance to minimise risks, and any issues are managed promptly.
-
5.Will PTBD or biliary stenting cure my jaundice permanently?
The procedure relieves the blockage and improves jaundice, but it does not cure the underlying cause (such as cancer or chronic stricture). Further treatment is planned in coordination with your treating hepatobiliary or oncology team.
-
6.How soon can other treatments begin after PTBD / stenting?
Once bilirubin and general condition improve, your doctors can proceed with surgery, chemotherapy or other planned treatments. The timing varies from patient to patient and is guided by repeat blood tests and clinical recovery.