Embolization Treatment for Bleeding Pseudoaneurysms
Embolization Treatment for Bleeding Pseudoaneurysms
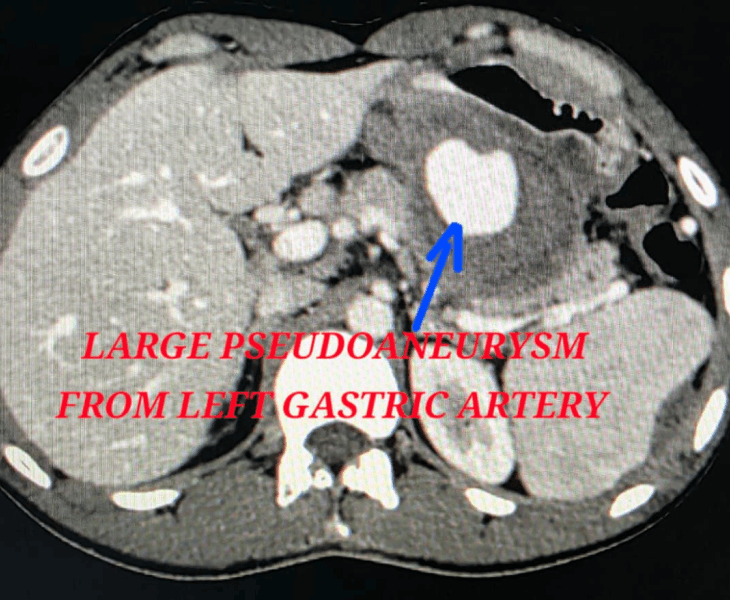
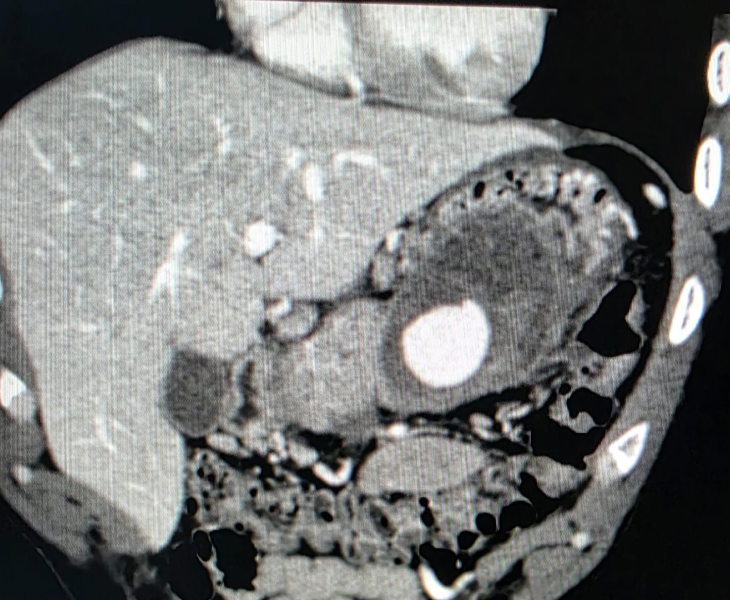
A pseudoaneurysm is a contained arterial bleed where blood escapes the artery through a tear and forms a sac outside the vessel wall. Unlike a true aneurysm, the sac is not made of normal artery wall, so it can rupture and cause severe internal bleeding.
Image‑guided embolization is a minimally invasive, life‑saving procedure that stops bleeding by blocking the injured artery from inside using coils or other embolic agents—often avoiding emergency surgery.
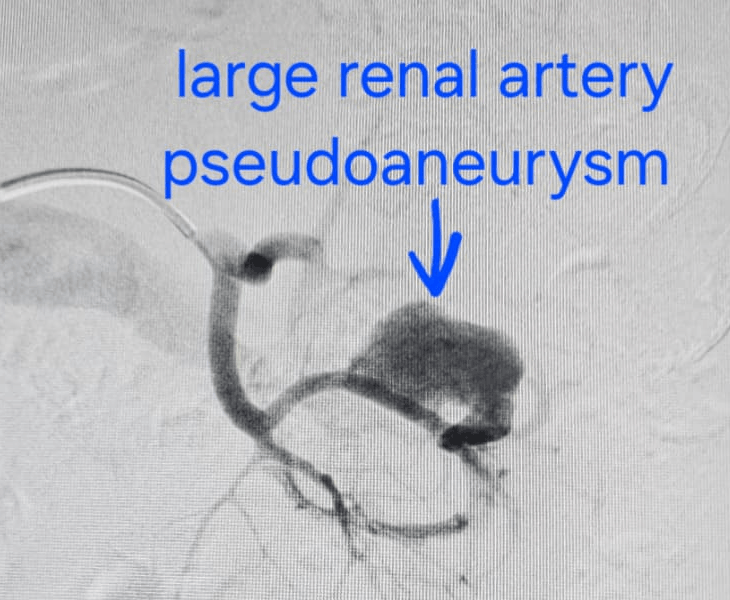
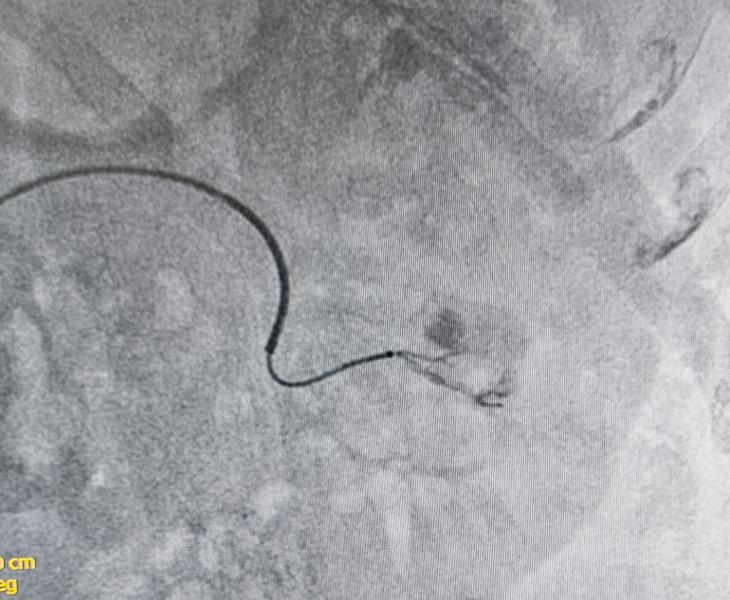
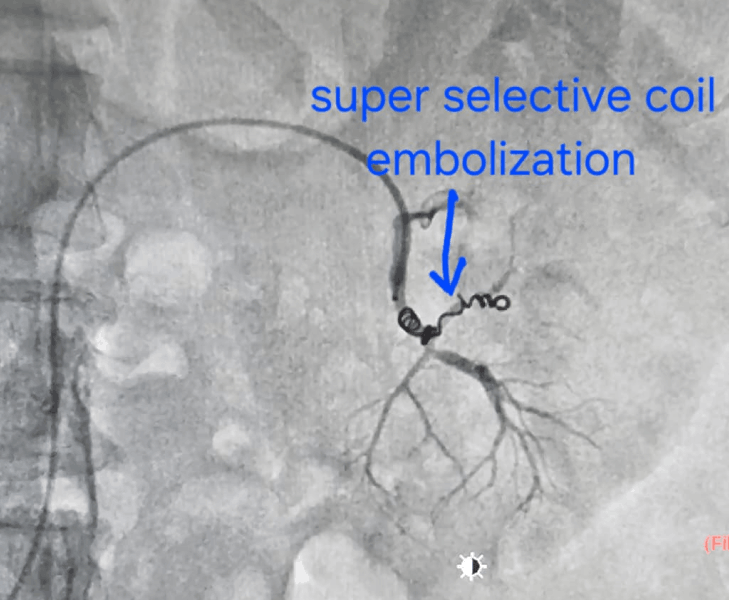
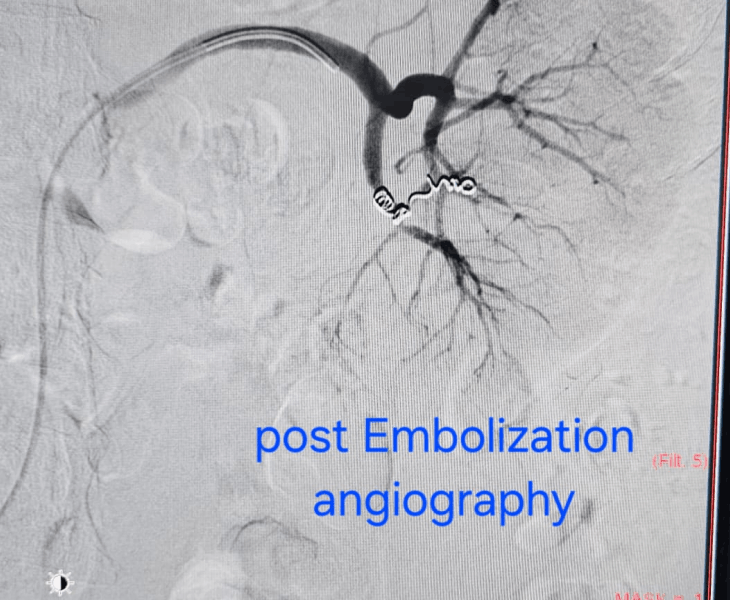
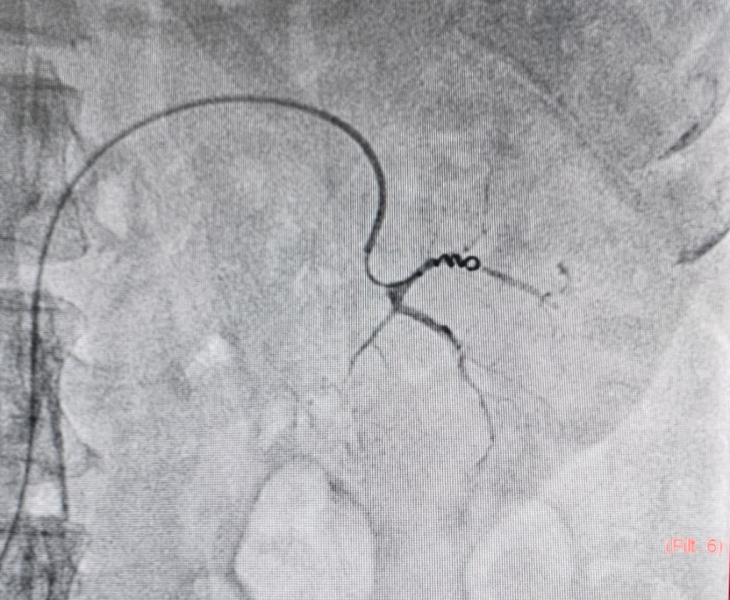
Why Pseudoaneurysms Need Urgent Treatment
Pseudoaneurysms can occur after trauma, surgery, procedures, pancreatitis or infection. Because they can rupture unpredictably, early diagnosis and prompt embolization is often the safest way to control bleeding.
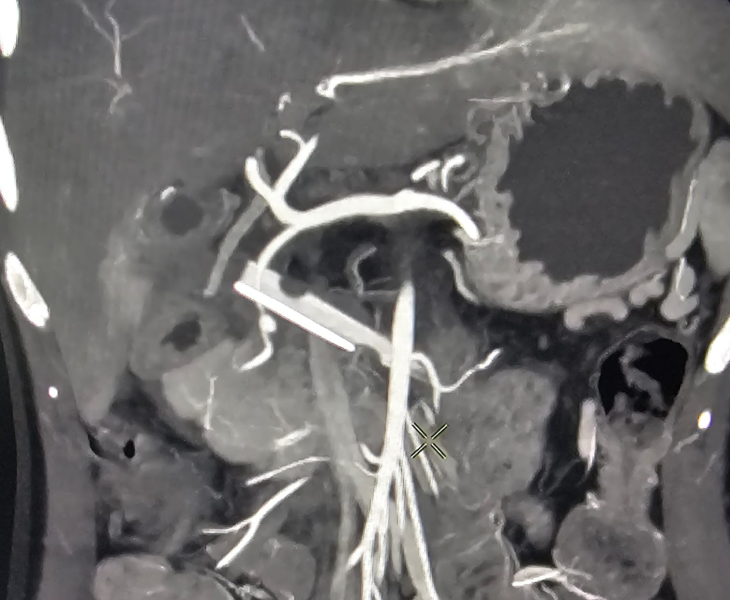
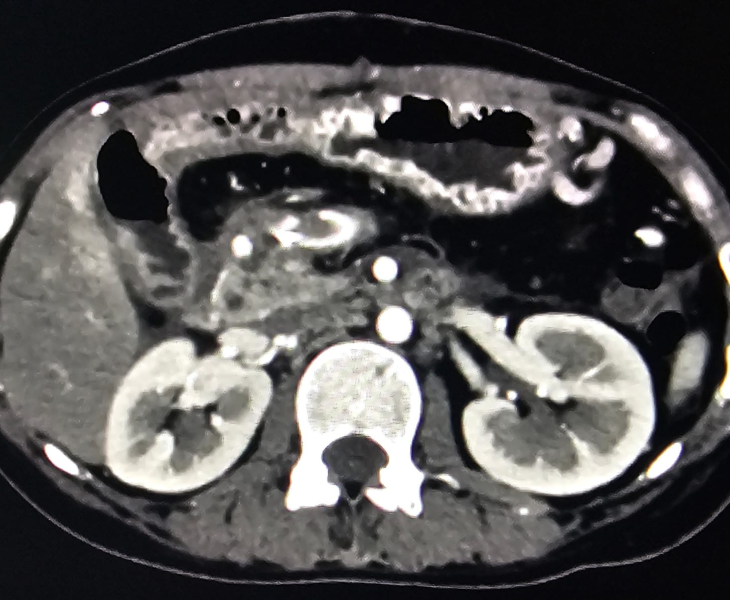
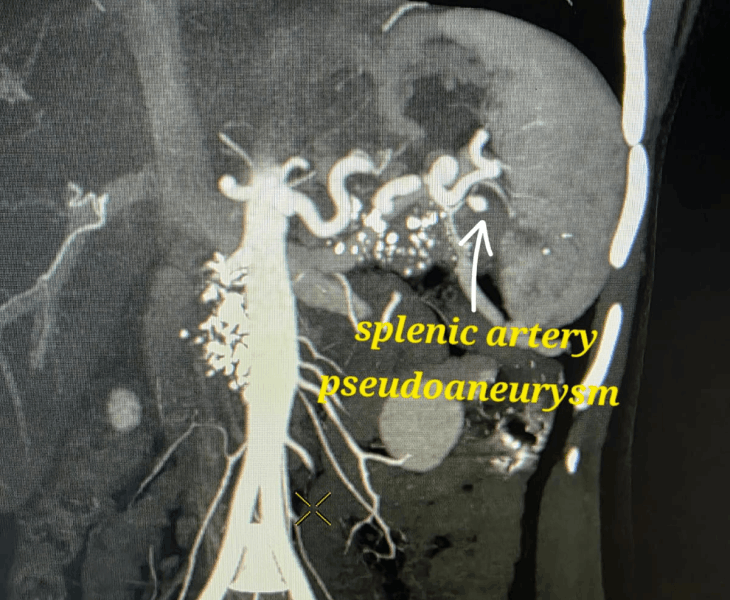
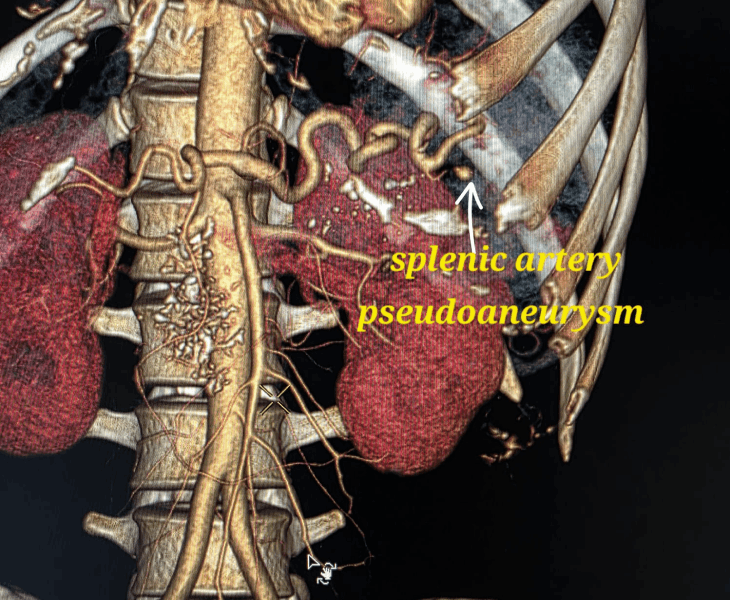
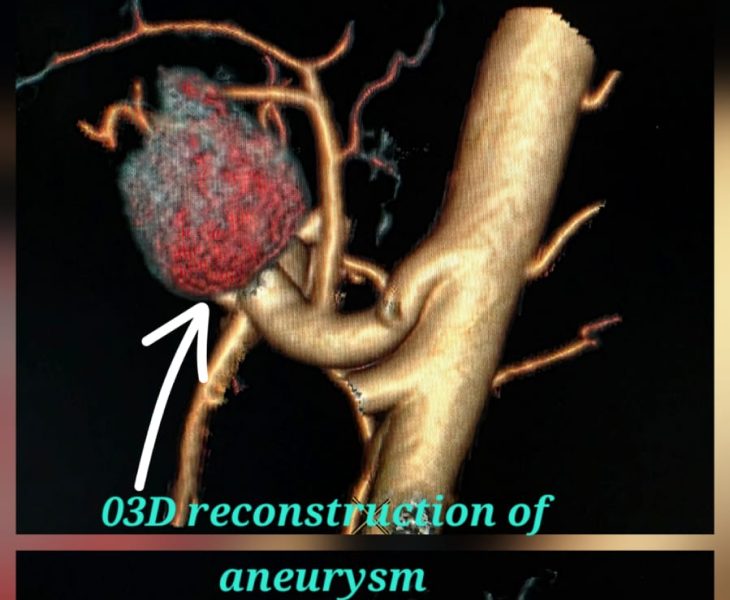
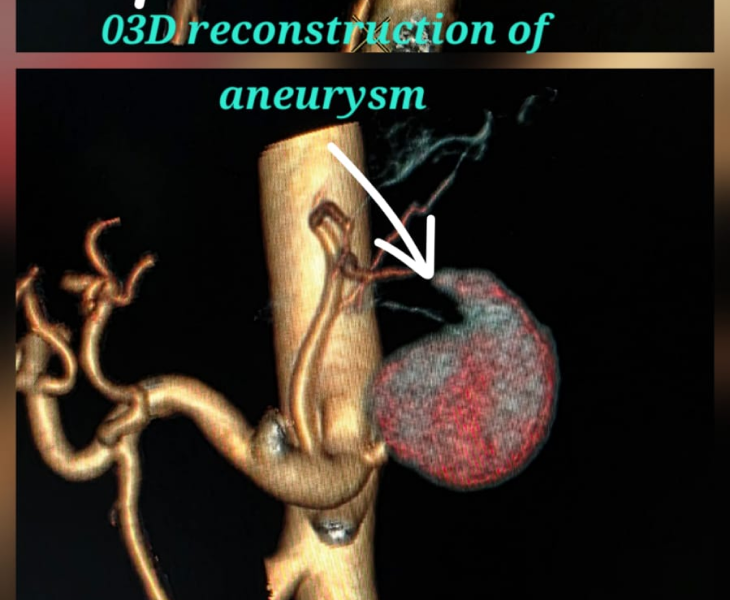
We use CT angiography and catheter angiography to identify the bleeding vessel precisely and then perform targeted embolization to seal it while preserving as much normal organ blood supply as possible.
Symptoms / Warning Signs
Symptoms depend on the organ involved, but common warning signs include:
- Sudden abdominal or flank pain
- Blood in vomit or black stools (gastrointestinal bleeding)
- Blood in urine (renal pseudoaneurysm)
- Dizziness, fainting, low blood pressure or shock
- Falling haemoglobin or unexplained anemia
- Bleeding after surgery or biopsy/procedure
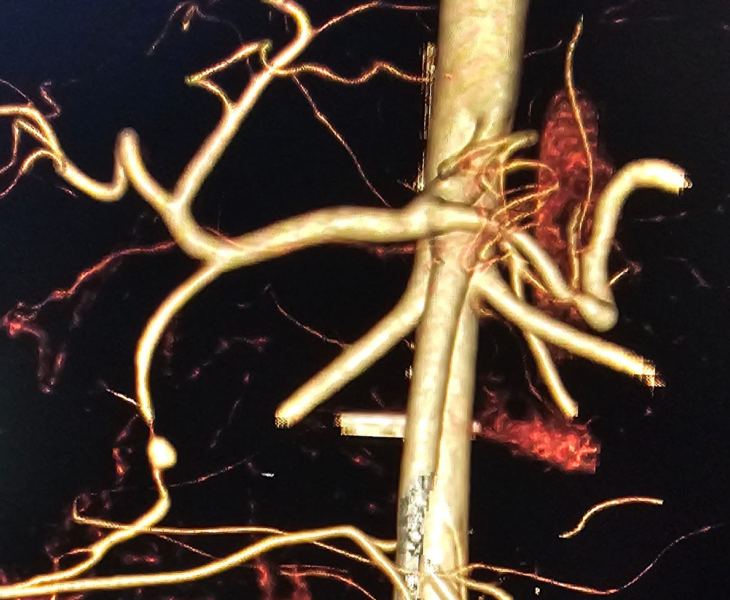
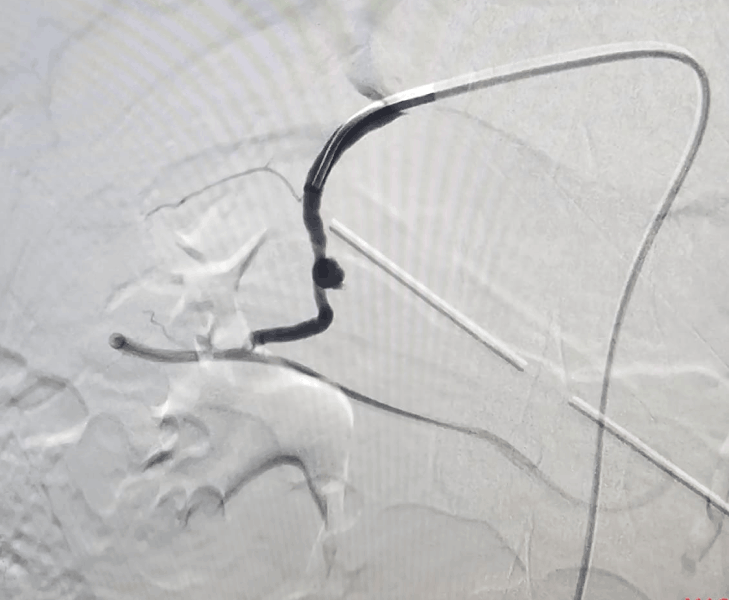
Treatment (Super‑Selective Embolization)
Embolization is performed in a catheterisation lab under fluoroscopy (X‑ray) guidance, usually through a tiny puncture in the groin or wrist artery.
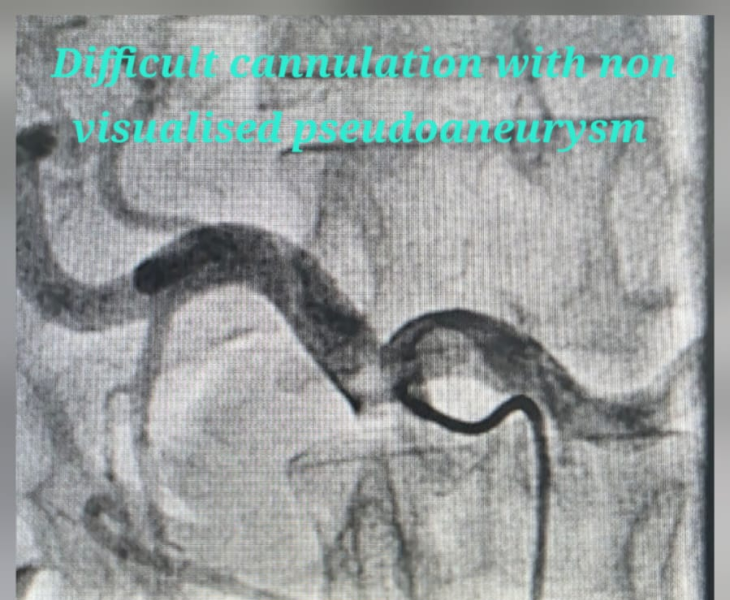
- Catheter angiography: contrast is injected to locate the pseudoaneurysm and bleeding source.
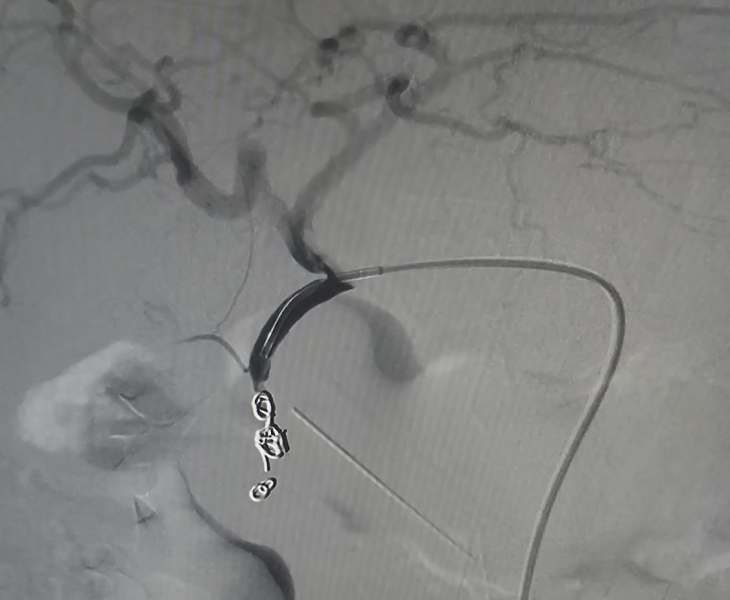
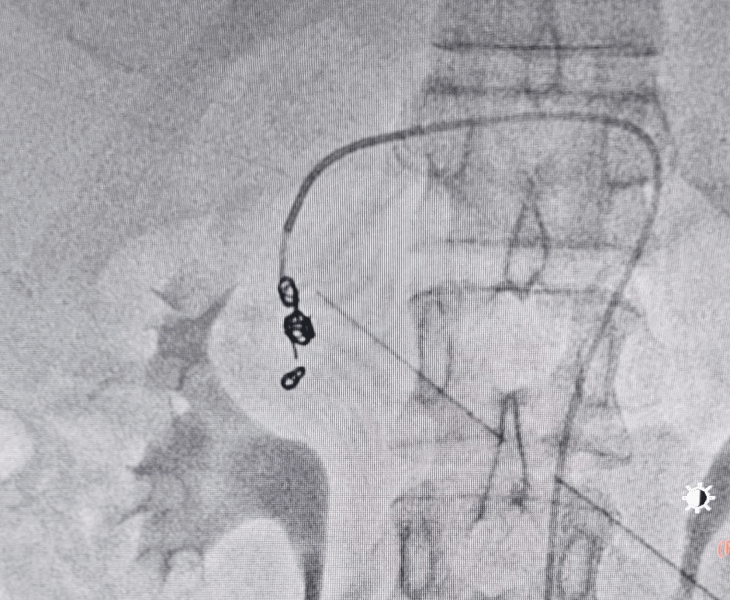
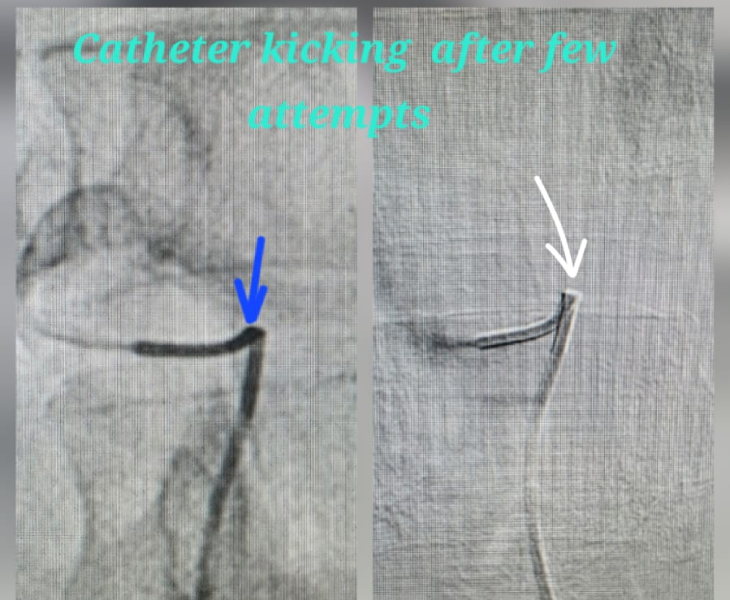
- Super‑selective catheterisation: a microcatheter is advanced into the specific branch feeding the pseudoaneurysm.
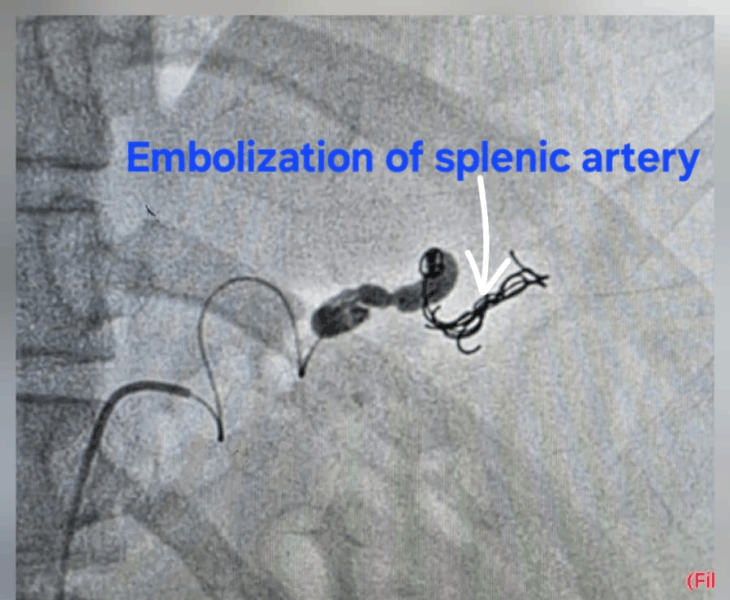
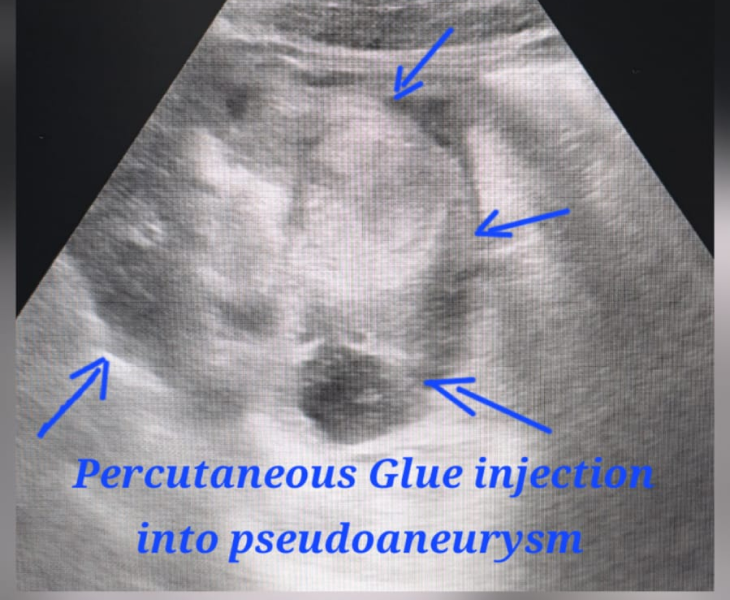
- Embolization: coils and/or other embolic agents are deployed to stop blood flow to the pseudoaneurysm.
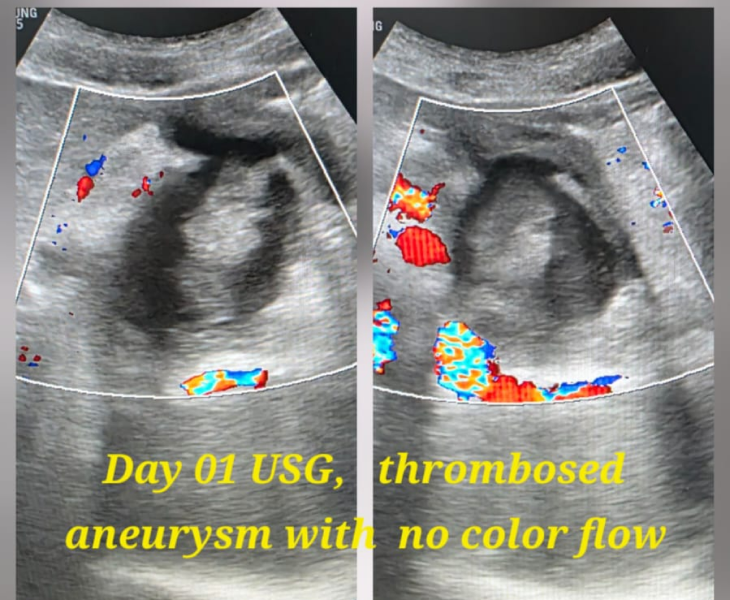
- Post‑embolization check: repeat angiography confirms complete sealing with preserved flow to normal tissues.
After Treatment
After embolization, patients are monitored closely to ensure bleeding control and stable recovery.
- Observation for pain, pulse, blood pressure and puncture‑site bleeding
- Repeat blood tests to check haemoglobin and organ function
- Hydration and medicines as advised (pain relief/antibiotics if needed)
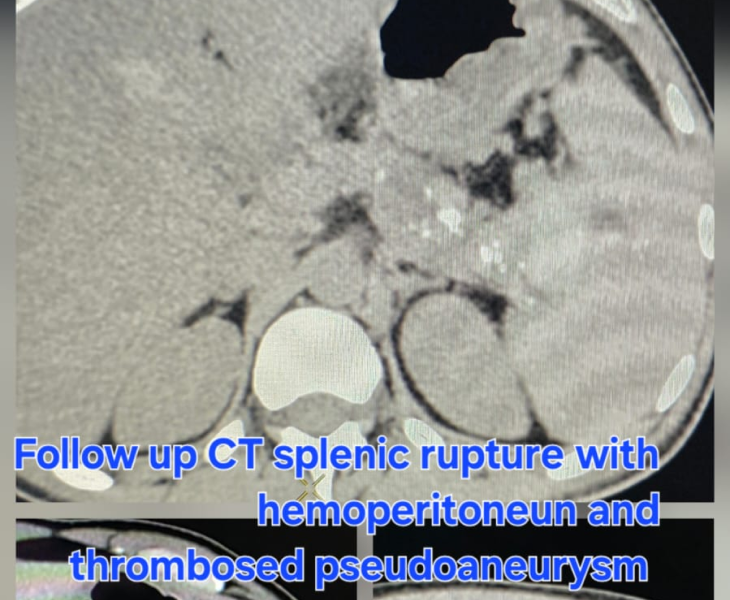
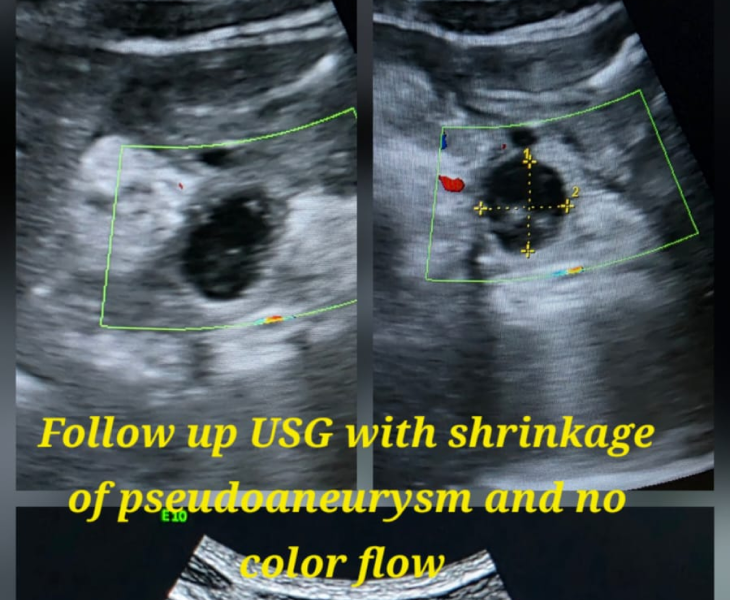
- Follow‑up imaging in selected cases to confirm durable occlusion
- Seek urgent care for fever, increasing pain, weakness or fresh bleeding
Frequently Asked Questions
-
1.What causes a pseudoaneurysm?
Pseudoaneurysms commonly occur after trauma, surgery or procedures (biopsy, catheterisation), and can also be caused by pancreatitis, infection or tumour‑related vessel erosion.
-
2.Is embolization safer than surgery?
In many cases, yes. Embolization treats the bleeding vessel through a tiny puncture without a large incision, and is especially useful in unstable patients or difficult‑to‑reach vessels. The best option depends on the location and your overall condition.
-
3.Will embolization affect organ function?
We use super‑selective techniques to block only the injured vessel branch while preserving normal blood supply. In rare cases, some tissue loss can occur, but the risk is usually much lower than uncontrolled bleeding or emergency surgery.
-
4.How long is the hospital stay?
It depends on the severity of bleeding and the underlying illness. Some patients may be discharged in 1–2 days, while others need longer monitoring if they were unstable or required transfusions.
-
5.Can a pseudoaneurysm recur after embolization?
Recurrence is uncommon but can occur if new collateral vessels develop or if the underlying cause persists. Follow‑up and repeat imaging may be advised based on the location and risk.
-
6.When should I seek emergency help?
Seek urgent care if you have sudden severe pain, dizziness/fainting, fresh bleeding (vomit/black stools/urine), fever, increasing weakness or swelling at the puncture site.