Cancer Treatment
Cancer Treatment Through Advanced Minimally Invasive Techniques
Interventional oncology offers targeted, minimally invasive options for many cancers. Using image guidance (ultrasound, CT, fluoroscopy), treatments are delivered directly to the tumour through tiny punctures, helping control disease while preserving healthy tissue.
These procedures are often performed as day-care or short-stay treatments, with smaller incisions, faster recovery, and the ability to combine with surgery, chemotherapy, or systemic therapies as part of a comprehensive cancer care plan.
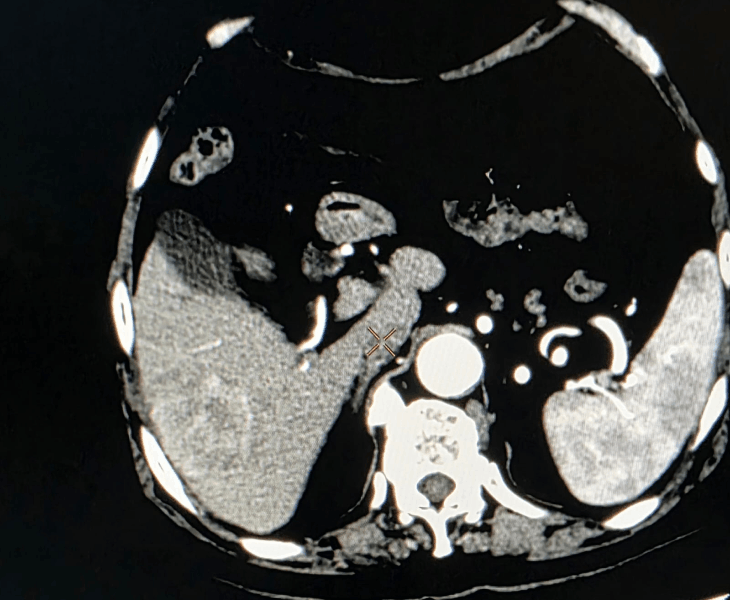
Microwave ablation of liver cancer
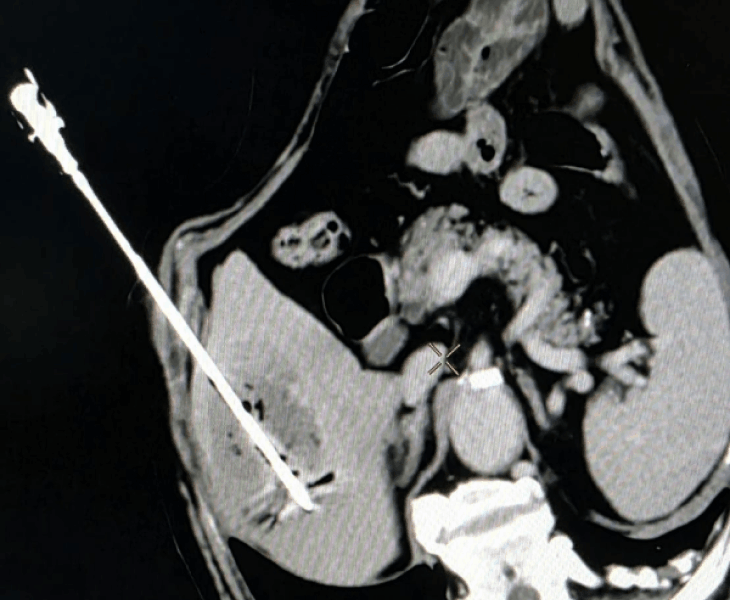
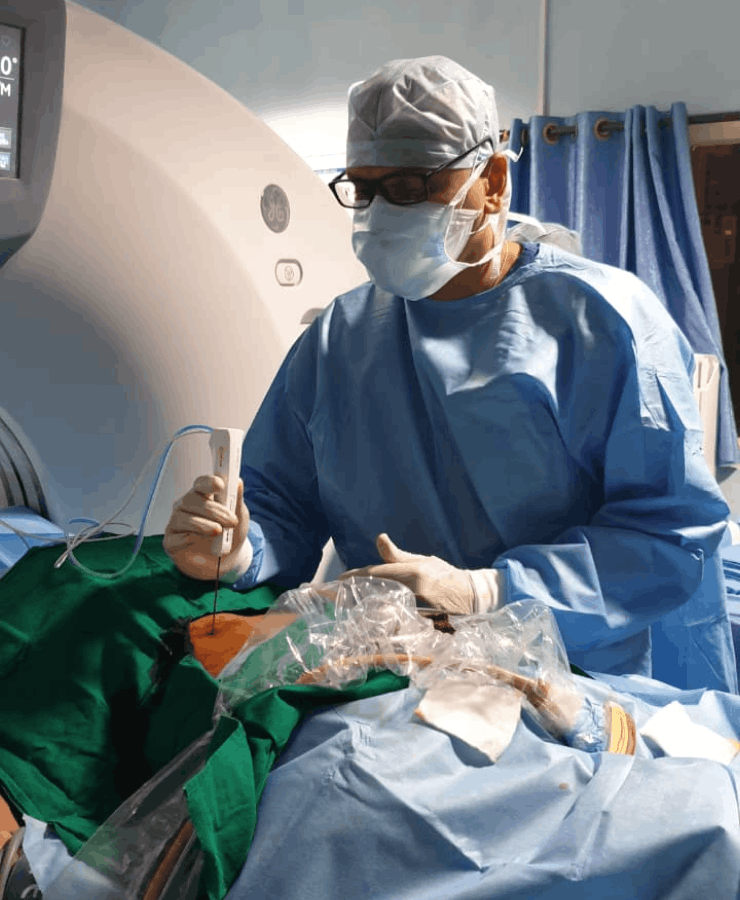
Insertion of microwave needle treatment of cancer
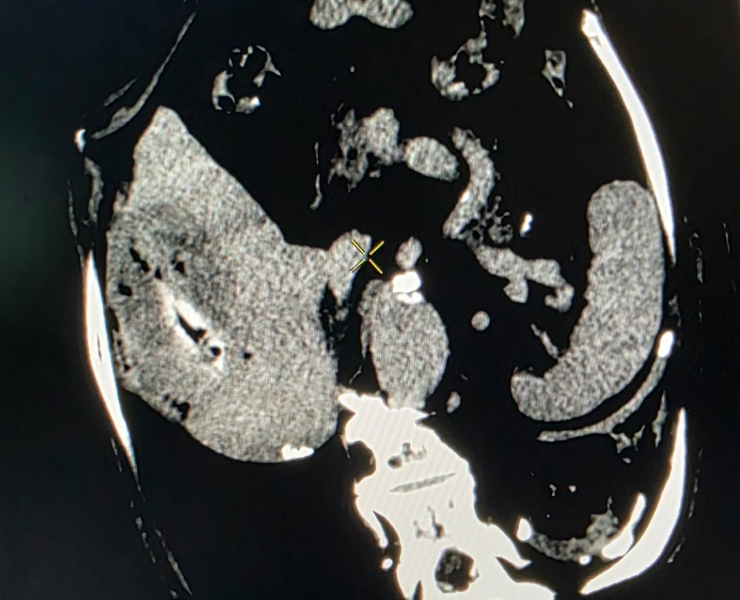
Post treatment
Cancer Treatment Through Advanced Minimally Invasive Interventional Techniques
Many liver and kidney cancer patients are not suitable for major surgery. For these patients, advanced interventional radiology procedures can treat tumours through tiny skin punctures, often under image guidance, with less pain, fewer complications, and quicker recovery.
We work in close coordination with your oncology and surgical teams. Each case is reviewed individually, and a personalised interventional plan is created based on tumour size, number, location, blood supply, and your general health.
Liver Cancer Treatment
Many liver cancer patients are not suitable for surgery because of tumour location, multiple lesions, underlying liver disease or general health. In such cases, interventional radiological procedures can offer effective, targeted options:
- Thermal ablation (radiofrequency or microwave): destroys tumour tissue by heating it from within through a thin needle placed under USG/CT guidance.
- Chemoembolization (TACE): delivers chemotherapy directly into the tumour’s blood supply, followed by embolic particles to block the vessels and cut off nutrition to the cancer.
- Combination strategies with systemic therapy or other liver-directed treatments as advised by the tumour board.
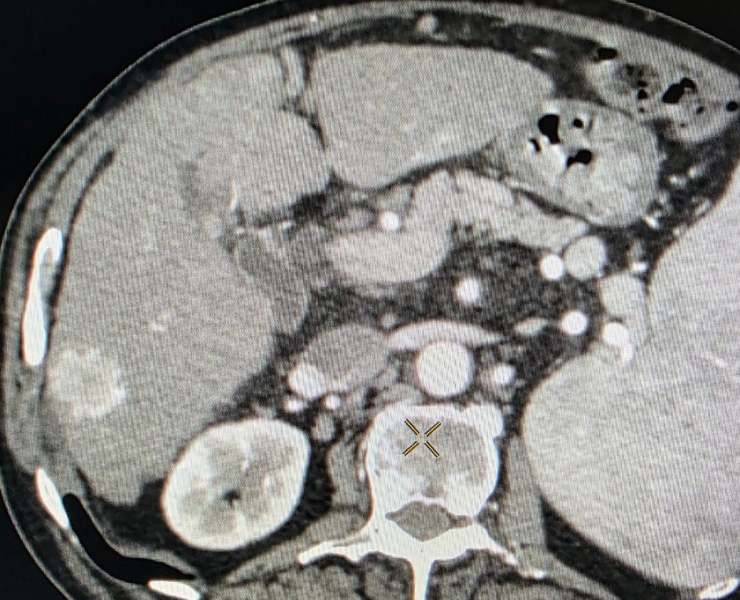
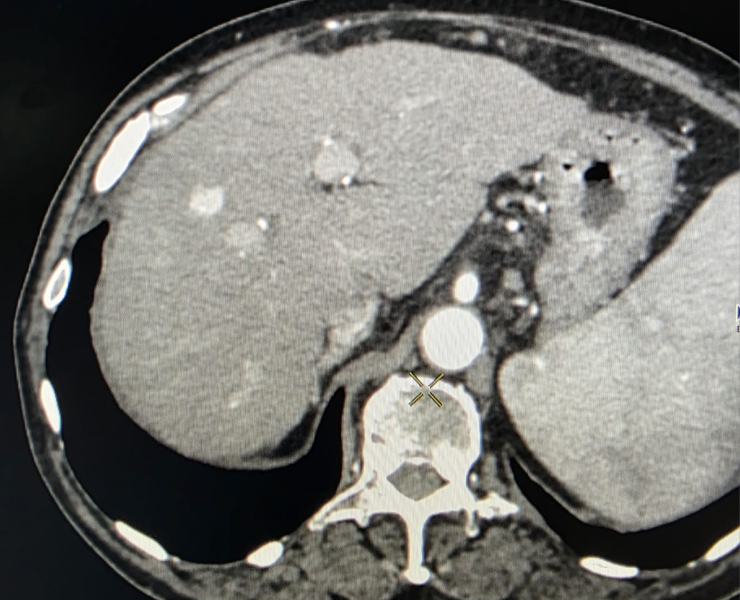
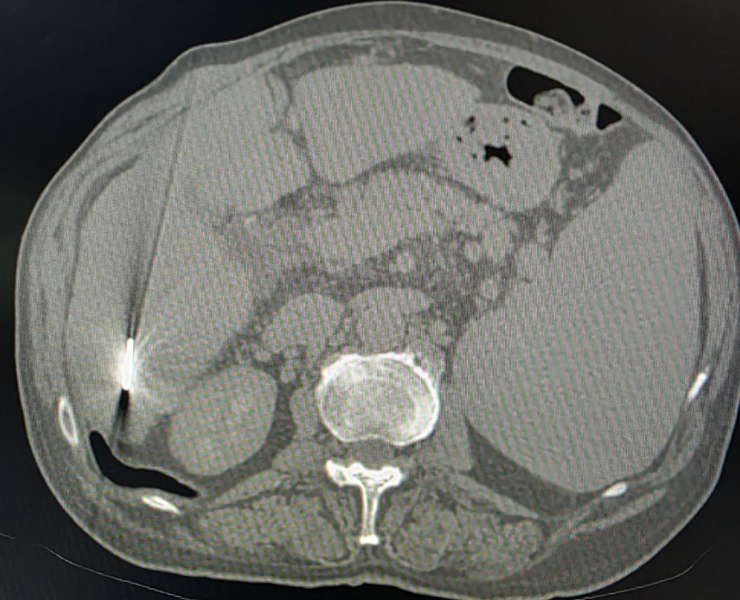
Microwave ablation of liver cancers
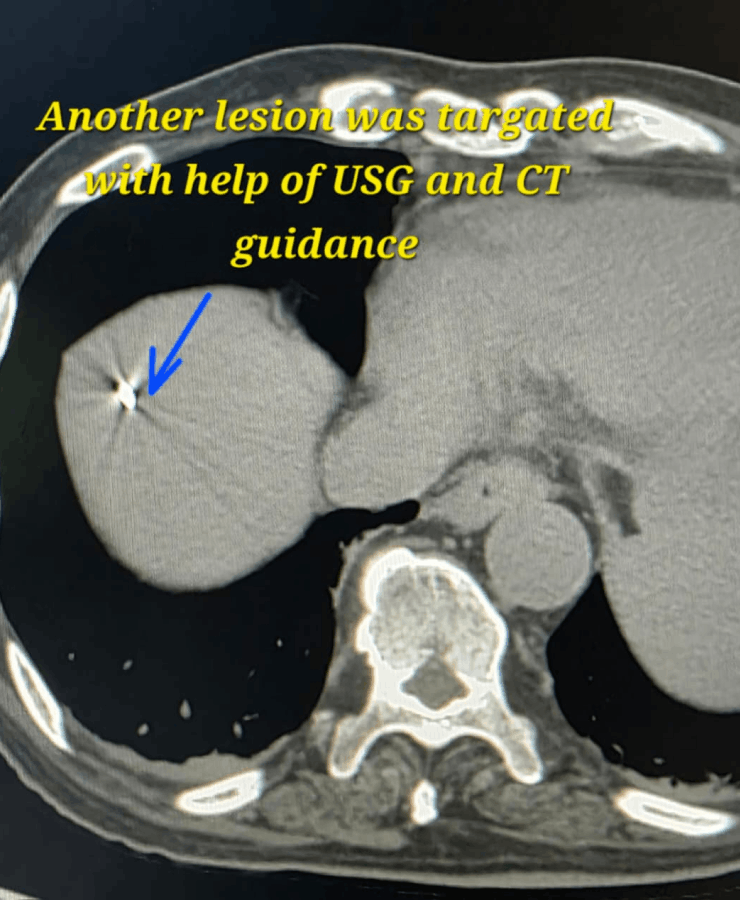
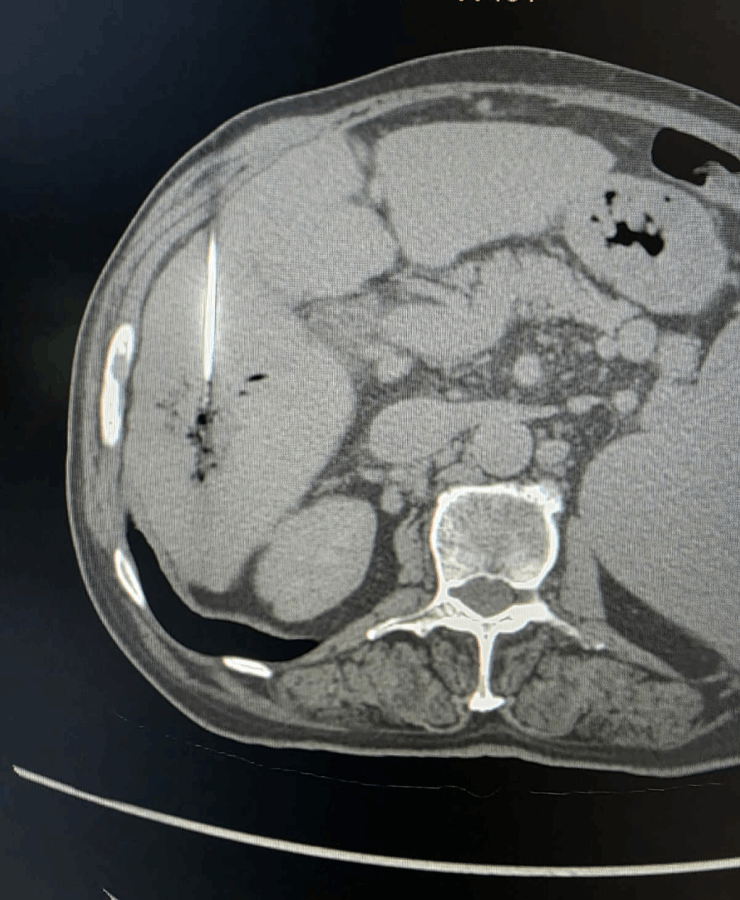
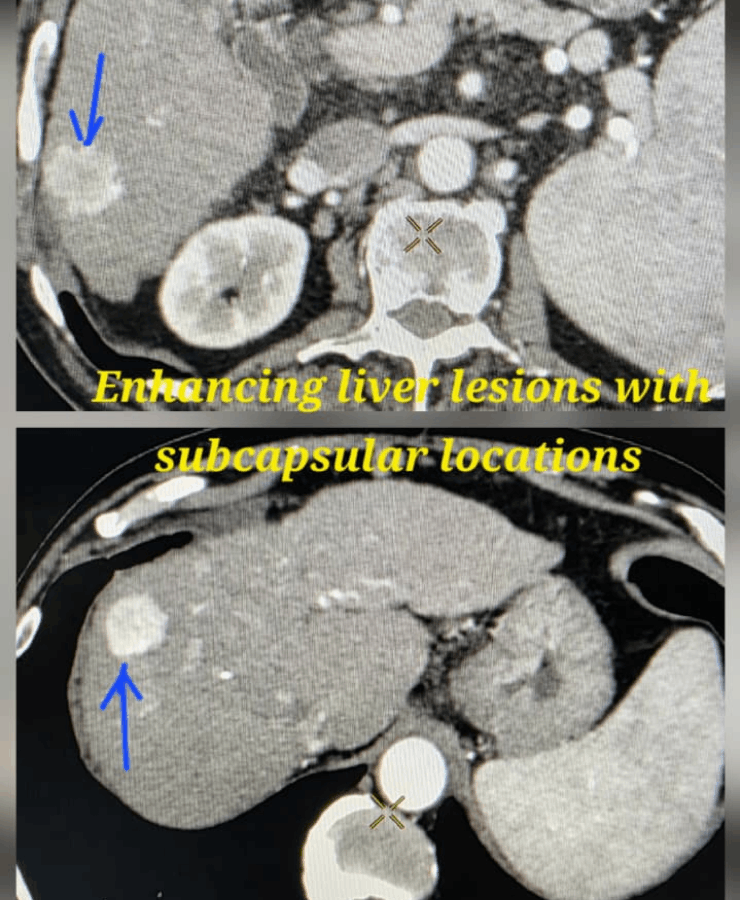
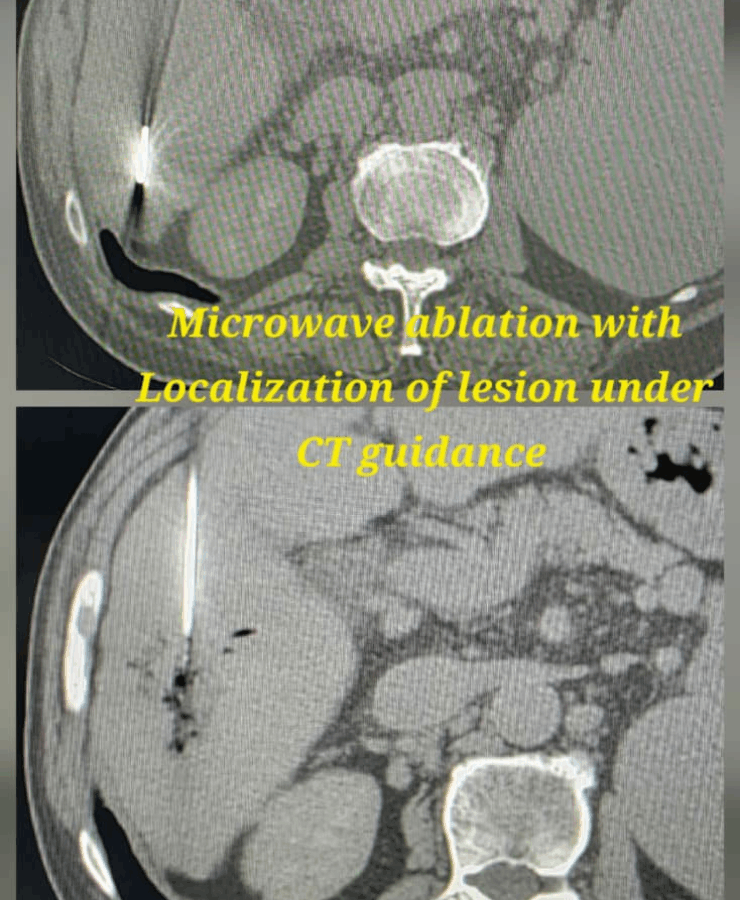
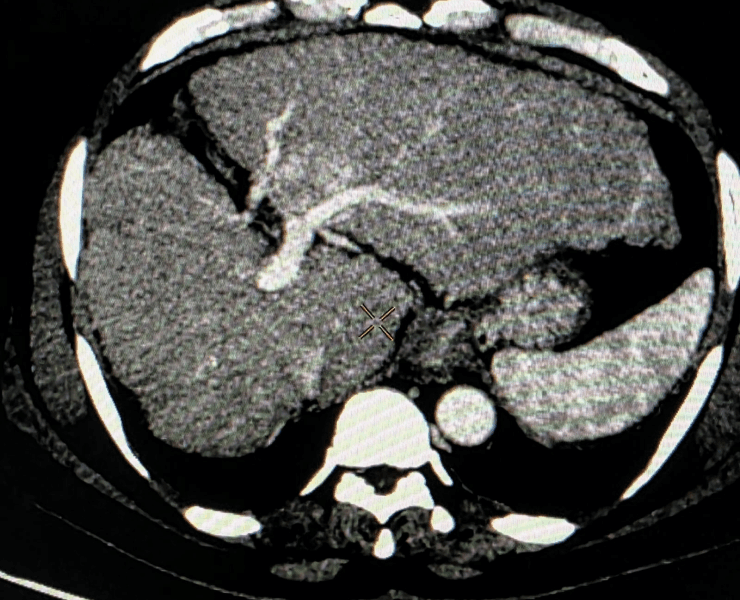
Liver tumor
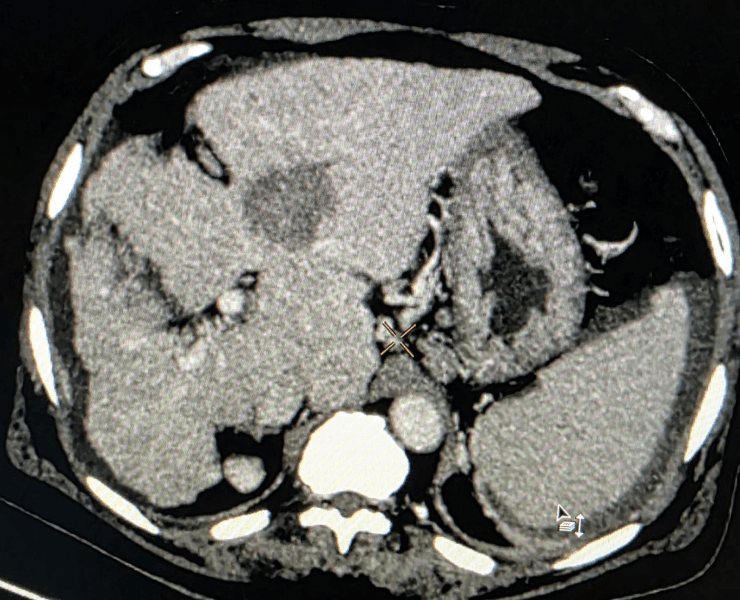
Post treatment (TACE) procedure
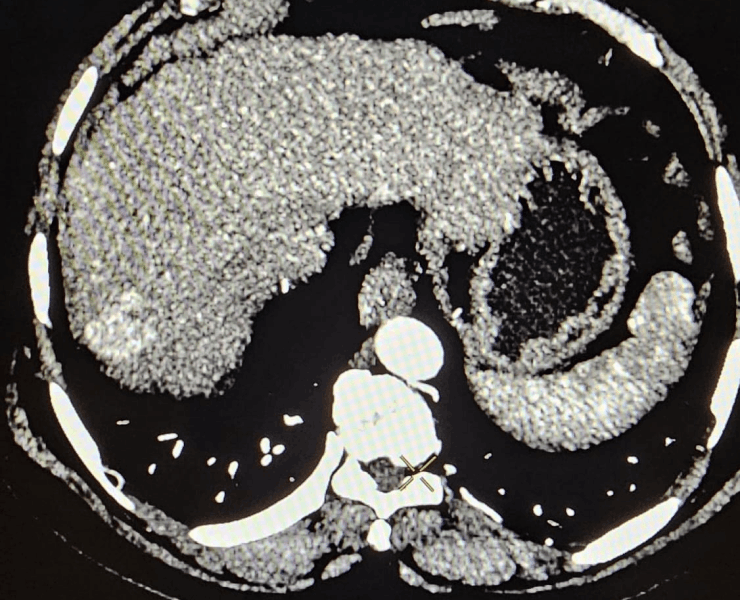
Before treatment liver cancer
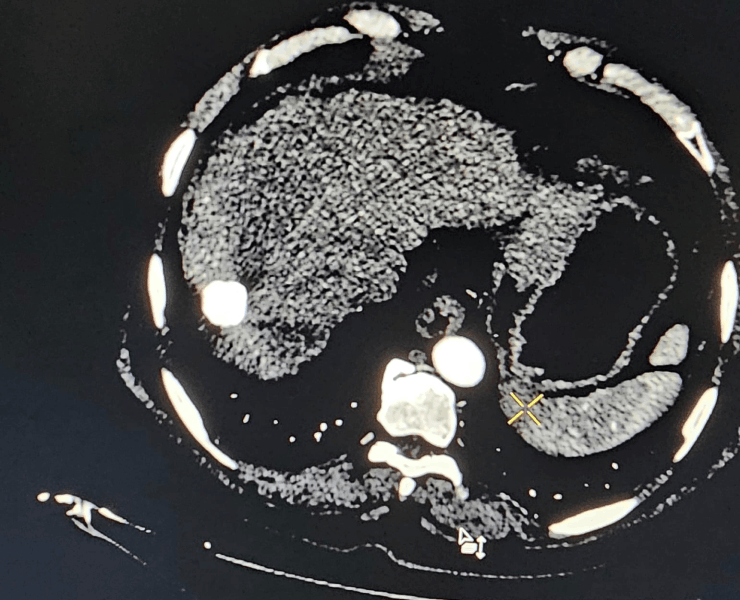
After treatment of liver cancer
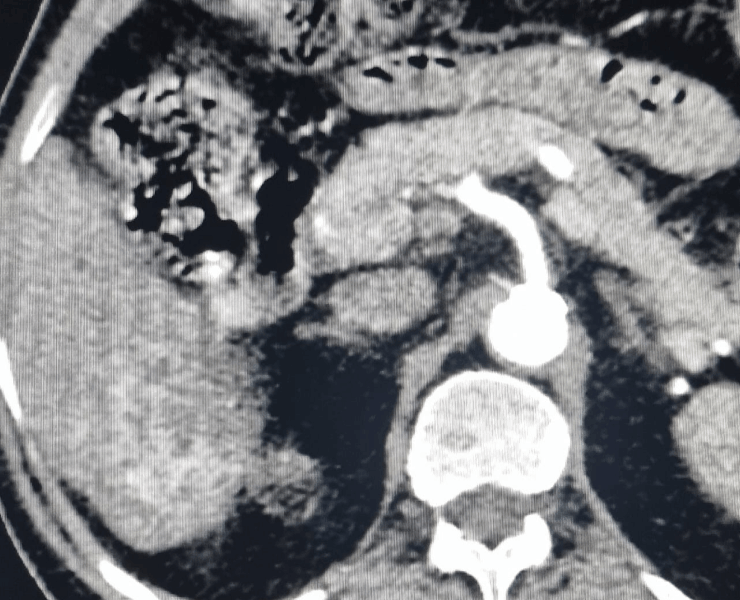
Chemoembolization of liver cancer before
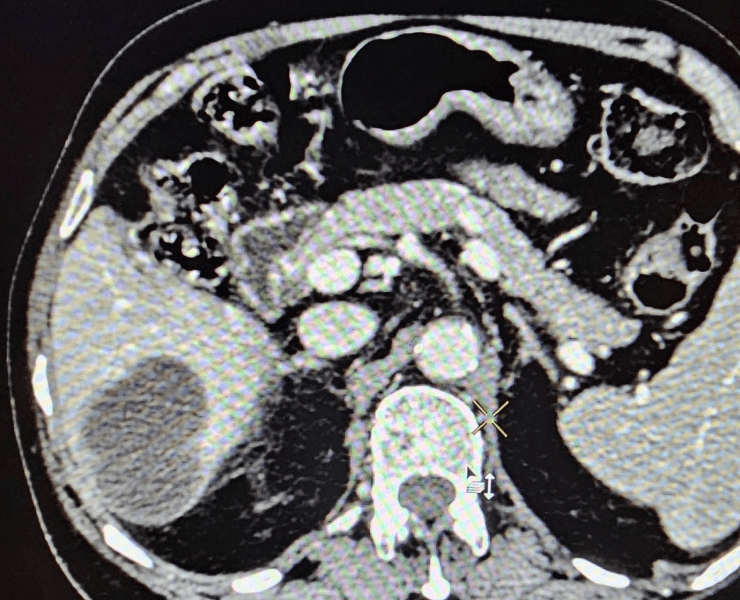
After treatment
Kidney Cancer Treatment
Many cancerous tumours of the kidney, especially small or localised lesions, can be treated by thermal ablation techniques rather than open surgery, depending on patient profile and tumour characteristics.
- Radiofrequency ablation (RFA): uses controlled radiofrequency energy to heat and destroy the tumour via a needle inserted through the skin.
- Microwave ablation: delivers microwave energy to achieve rapid, predictable ablation zones, often suitable for selected renal tumours.
- Procedures are performed under USG/CT guidance to precisely target the lesion while preserving as much normal kidney tissue as possible.
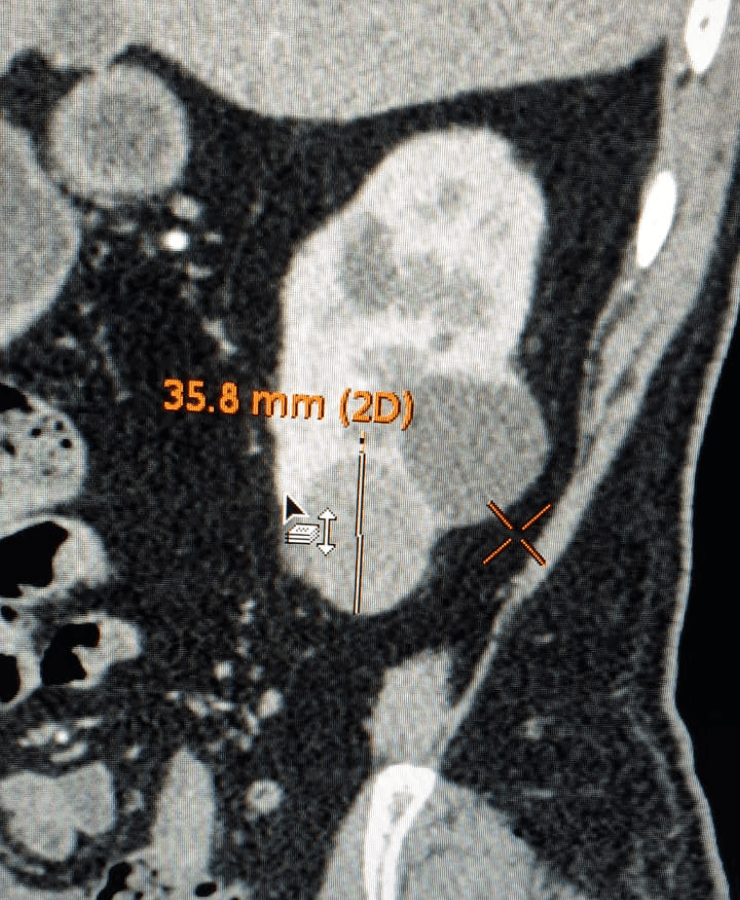
Kidney cancer treatment by Microwave Ablation method
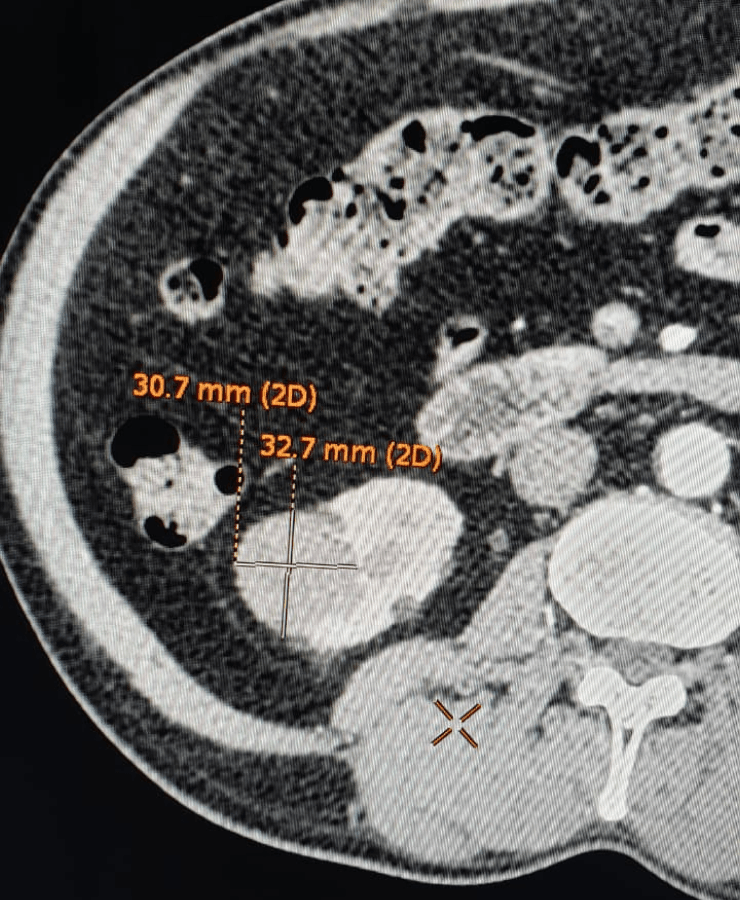
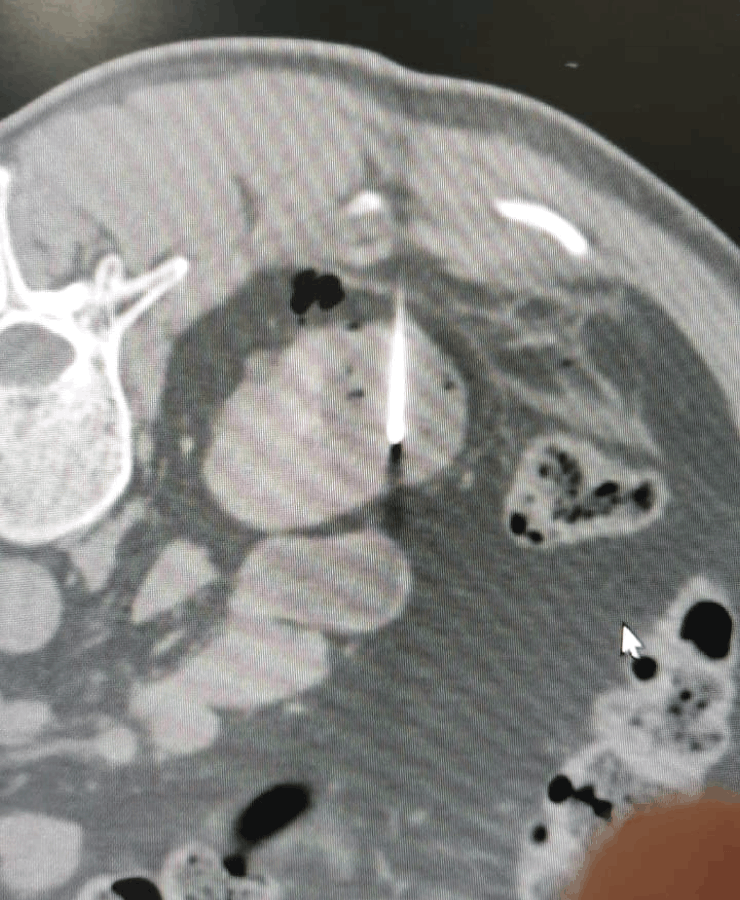
Post treatment
Frequently Asked Questions
-
1.Who is a candidate for interventional cancer treatment?
Patients with liver or kidney tumours who are not ideal candidates for major surgery, or who need tumour control while awaiting or combining other therapies, may benefit. Suitability is decided after imaging, lab evaluation and multidisciplinary discussion.
-
2.Are these procedures done under general anesthesia?
Many interventional oncology procedures are performed under conscious sedation and local anesthesia, though some may require general anesthesia depending on tumour location, duration and your overall health.
-
3.How long will I need to stay in the hospital?
Some treatments are day-care procedures with discharge the same day, while others may need an overnight stay for observation and pain control. Your doctor will discuss the expected hospital stay before the procedure.
-
4.Can interventional procedures cure my cancer?
For small, well-selected tumours, ablation can sometimes achieve results comparable to surgery. In other cases, the aim is to shrink or control the cancer, relieve symptoms and improve quality of life as part of a broader treatment plan.
-
5.What are the possible risks or side effects?
All procedures carry some risk, such as pain, bleeding, infection, post-embolization syndrome (fever, fatigue, discomfort) or injury to nearby structures. We perform detailed evaluation and imaging to minimise these risks and monitor you closely after treatment.
-
6.How will my follow-up be planned after the procedure?
You will receive a clear follow-up schedule for clinic visits, imaging scans and blood tests. The results are shared with your treating oncologist/surgeon so that your overall cancer care plan remains coordinated and up to date.